Therapeutic And Expert Insights into OCD: Effective Treatments, Symptoms, and Modern Interventions
Introduction to Therapeutic And Expert Insights into OCD
Obsessive-Compulsive Disorder (OCD) is a challenging and often misunderstood mental health condition. Many people imagine it as a desire for neatness or perfection, but OCD runs much deeper. It can affect relationships, work, school, and everyday tasks. This article offers clear, research-based Therapeutic And Expert Insights into OCD, making it easier to understand symptoms, causes, and proven treatments.
With guidance from mental health experts, individuals can learn to manage OCD successfully, rebuild confidence, and regain control over their lives.
Understanding Obsessive-Compulsive Disorder (OCD)
Defining Obsessions and Compulsions
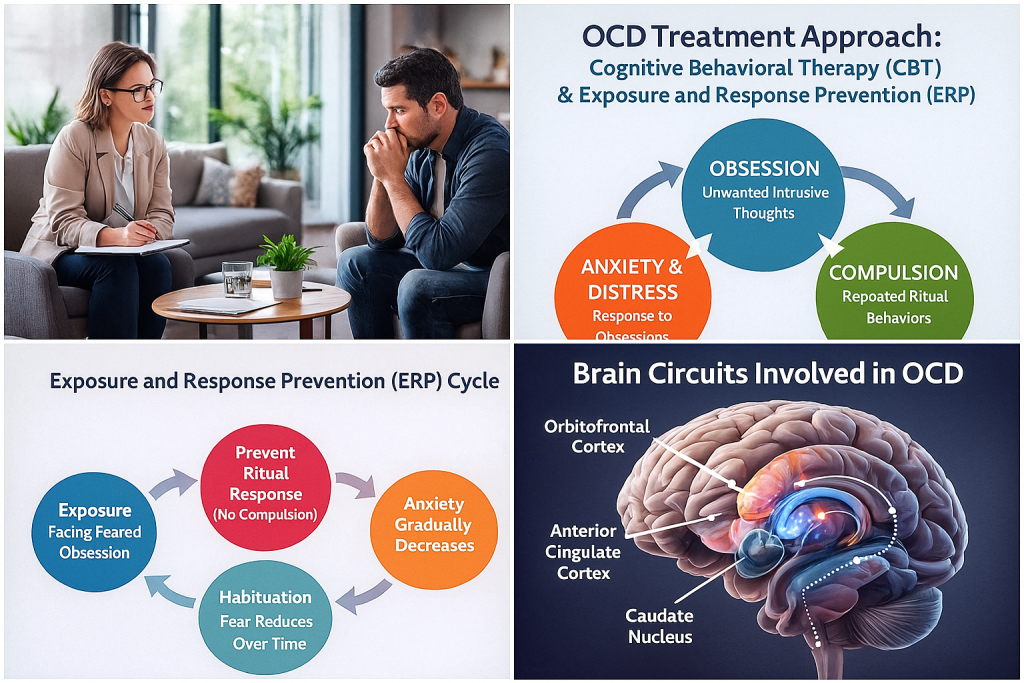
OCD includes two main parts:
Obsessions: unwanted, intrusive thoughts, images, or urges
Compulsions: actions or mental rituals done to reduce anxiety
These can form strong cycles that feel impossible to break.
Common Misconceptions About OCD
Many assume OCD is about being clean or organized. In reality, OCD can involve fears about harm, contamination, mistakes, morality, or even one’s identity.
Subtypes and Variations
Some common forms include:
Contamination OCD
Checking OCD
Pure O (intrusive thought-based OCD)
Relationship OCD
Perfectionism OCD
Causes and Contributing Factors
OCD doesn’t have a single cause. Instead, experts believe it results from a mix of influences.
Genetic Influences
Research shows OCD can run in families, suggesting a hereditary link.
Neurological Differences
Brain scans show that people with OCD often have overactive fear and decision-making circuits.
Environmental and Developmental Triggers
Stress, trauma, or major life changes can activate OCD symptoms in susceptible individuals.
How OCD Affects the Brain
Role of the CSTC Loop
The cortico-striato-thalamo-cortical (CSTC) loop regulates decision-making and threat detection. In OCD, this loop becomes overactive, creating constant “false alarms.”
Serotonin and Dopamine Imbalances
Experts believe OCD is connected to serotonin imbalances, which is why certain medications help stabilize symptoms.
Therapeutic And Expert Insights into OCD Treatment Approaches
This is where expert guidance becomes incredibly powerful. The most effective treatments teach individuals to break obsessive cycles and face fears gradually.
Cognitive Behavioral Therapy (CBT)
CBT helps people challenge distorted thoughts and build healthy coping skills.
Exposure and Response Prevention (ERP)
Widely considered the gold standard treatment, ERP exposes individuals to their fears while preventing compulsive behaviors. Over time, the brain learns the fear is manageable.
Acceptance and Commitment Therapy (ACT)
ACT teaches individuals to accept intrusive thoughts without giving them power, allowing them to focus on personal values.
Mindfulness-Based Interventions
Mindfulness helps individuals sit with discomfort, reduce stress, and separate thoughts from identity.
Medication Options for OCD
SSRIs and SNRIs
Medications like fluoxetine, sertraline, and fluvoxamine help regulate serotonin levels. They are often prescribed at higher doses for OCD.
Off-Label Medication Treatments
In some cases, doctors use medications such as clomipramine or antipsychotic augmentations to support symptom reduction.
When Therapy and Medication Are Combined
Benefits of Integrated Treatment
Many people see the best results when medication reduces symptoms enough for ERP and CBT to be more effective.
Case Example of Combined Therapy
A young adult with checking OCD may use SSRIs to lower anxiety, allowing them to participate fully in exposure exercises.
Advanced and Emerging Treatments
Deep Brain Stimulation (DBS)
DBS helps individuals with severe, treatment-resistant OCD by modulating brain activity.
Transcranial Magnetic Stimulation (TMS)
TMS targets specific brain circuits using magnetic pulses.
Digital Therapeutics and Online ERP Programs
Modern apps and telehealth platforms make therapy more accessible than ever.
Lifestyle and Self-Help Strategies
Stress Management Tools
Breathing exercises, journaling, and grounding techniques help calm the nervous system.
Sleep, Nutrition, and Exercise
Healthy routines improve mood, clarity, and resilience.
Support Groups and Family Education
Connecting with others can relieve isolation and offer hope.
Working with OCD in Children and Teens
Early Detection
Children may show signs like excessive reassurance seeking or repetitive “just-right” behaviors.
Therapy Adaptations for Youth
ERP is adjusted using playful exposures, reward systems, and family involvement.
Expert Tips for Family Members and Caregivers
Reducing Accommodation
Family members often unintentionally support compulsions. Experts teach families how to step back while still offering support.
Healthy Supportive Behaviors
Encouragement, consistency, and calm communication are essential.
Myths vs. Facts About OCD
| Myth | Fact |
|---|---|
| “OCD is just being neat.” | OCD involves distressing intrusive thoughts, not preference. |
| “People can stop if they try harder.” | OCD requires structured treatment, not willpower. |
| “OCD is rare.” | Millions of people worldwide live with OCD. |
Frequently Asked Questions
1. What is the most effective treatment for OCD?
ERP is the gold standard, often combined with CBT and medication.
2. Can OCD go away on its own?
OCD typically requires structured treatment, but symptoms can greatly improve with therapy.
3. Are intrusive thoughts normal?
Everyone has intrusive thoughts, but people with OCD misinterpret them, causing distress.
4. Do kids get OCD?
Yes. OCD can appear as early as age 6 or 7.
5. How long does treatment take?
ERP often shows results within 12–20 sessions, though ongoing support varies.
6. Where can I learn more?
A helpful resource is the International OCD Foundation (IOCDF).
Conclusion
Understanding OCD is the first step toward transformation. With strong Therapeutic And Expert Insights into OCD, individuals can recognize symptoms earlier, seek proven treatments, and regain control of their lives. Through ERP, CBT, medication, and lifestyle tools, recovery becomes not only possible—but empowering.